Three Steps Forward, Two Steps Back
The Continued Struggle to Treat Mental Illness in America
Picture a maze. The first steps in the path may start off clear and confident, but soon they hit a wall or false turn and must retreat and reevaluate. As with a maze, the response to mental illness throughout history has seen shifts and turns of imperfect progress.
This exhibit explores both societal and medical treatments of mental illness in the US from the 18th century to today. It highlights institutional confinement, medical and pharmaceutical treatments, the development of child psychiatry, and the shift to police as mental illness first responders. Patterns of advancement and retreat carry through each case, showing the struggle to properly treat mental illness continues today.
Location: Eckenhoff Reading Room
Dates: Feb. 5 to July 31, 2026
Contact: ghsl-special
This exhibit was created to complement the National Library of Medicine’s traveling exhibit, Care & Custody: Past Responses to Mental Health, on display in the Galter Library atrium February 9 - March 21, 2026.
Events
Galter Library hosted several events in conjunction with this exhibit and the NLM exhibit.
- Curator Tour of the exhibit: Tuesday, February 24, 12-1pm; Thursday, March 19, 11am-12pm; and Tuesday, April 14, 12-1pm.
- Special Collections Open House: Tuesday, March 3, 11am - 4pm. The Special Collections Reading Room is located on the second floor, at the top of the stairs (Room 2-411).
- Exhibit of memoirs written by people hospitalized for mental illness in Dollie’s Corner, available to check out. Curated by Lindsey O’Brien.
- Art activities in our craft corner, February 2026.
Credits
Curated by Emma Florio, MLIS, Archives & Research Specialist; Katie Lattal, MA, Special Collections Librarian; Corinne Miller, MLIS, Clinical Librarian; Lindsey O’Brien, MSLIS, Cataloging & Metadata Librarian; and Annie Wescott, MLIS, Research Librarian.
Designed by Katie Lattal and Emma Florio.
Bibliography
Moral Treatment
- Bockover, J. Sanbourne. Moral Treatment in American Psychiatry. New York: Springer Publishing Company, 1963. https://research.ebsco.com/linkprocessor/plink?id=e3108f00-7fb2-31d2-bb08-ed6c947c17f2
- Bucknill, J.C., and D.H. Tuke. A Manual of Psychological Medicine... 4th ed. London: J. & A. Churchill, 1879. https://catalog.hathitrust.org/Record/001587747
- Burdett, Henry C. Hospitals and Asylums of the World: Their Origin, History, Construction, Administration, Management, and Legislation. London: J. & A. Churchill, 1891. https://catalog.hathitrust.org/Record/001581280
- Grob, Gerald N. Mental Institutions in America: Social Policy to 1875. New York: Free Press, 1972.
- Grob, Gerald N. Mental Illness and American Society, 1875-1940. Princeton: Princeton University Press, 1983. https://www.fulcrum.org/concern/monographs/8623hz10x
- Hogarth, William. “Plate 8 (Tom Rakewell Ends up in the Bethlehem Hospital Madhouse)” from A Rake’s Progress. Etching and engraving. 1735. https://risdmuseum.org/art-design/collection/plate-8-tom-rakewell-ends-bethlehem-hospital-madhouse-522288
- Kirkbride, Thomas S. On the Construction, Organization and General Arrangements of Hospitals for the Insane. Philadelphia: Lindsay & Blakiston, 1854. https://catalog.hathitrust.org/Record/008595368
- Mehr, Joseph. An Illustrated History of Illinois Public Mental Health Services, 1847 to 2000. Victoria, B.C.: Trafford Publishing, 2002.
- Tinworth, Joanna. “A Rake’s Progress VIII: The Madhouse.” Sir John Soane’s Museum Collection Online. 2021. https://collections.soane.org/object-p47
- Tuke, Samuel. Description of the Retreat, an Institution near York, for Insane Persons of the Society of Friends... York: W. Alexander, 1813. https://wellcomecollection.org/works/dcy3yd8x
- Tuke, Samuel. Practical Hints on the Construction and Economy of Pauper Lunatic Asylums. York: William Alexander, 1815. https://archive.org/details/39002011122984.med.yale.edu/
- Western Bank Note & Engraving Co. “Illinois Northern Hospital for the Insane.” Engraving. Chicago. From Tucker, G.A. Lunacy in Many Lands... n.p., [1885?]. https://catalogue.nla.gov.au/catalog/2438921
Children and Adolescents
- Addams, Jane. “The Bad Boy of the Street.” Ladies’ Home Journal 26 (October 1909): 17, 76. https://babel.hathitrust.org/cgi/pt?id=mdp.39015011414250&seq=322
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 2nd ed. Washington, DC: American Psychiatric Association, 1968. https://www.madinamerica.com/wp-content/uploads/2015/08/DSM-II.pdf
- Brierre de Boismont, A. “On the Insanity of Early Life.” Journal of Psychological Medicine and Mental Pathology 10, no. 8 (1857): 622–638. https://pmc.ncbi.nlm.nih.gov/articles/PMC5091123/
- Department of Psychiatry. "History." University of Illinois Chicago. n.d. Accessed January 7, 2026. https://www.psych.uic.edu/about-us/history
- Gingell, Kate. “The Forgotten Children: Children Admitted to a County Asylum between 1854 and 1900.” Psychiatric Bulletin of the Royal College of Psychiatrists 25, no. 11 (2001): 432–434. https://doi.org/10.1192/pb.25.11.432
- Healy, William. “A Pictorial Completion Test.” Psychological Review 21, no. 3 (1914): 189–203. https://doi.org/10.1037/h0075712
- Hull-House Photograph Collection. University of Illinois Chicago. Accessed January 7, 2026. https://digital.library.uic.edu/view/ark:/81984/d3vd6pc7j
- "Illinois Supreme Court History: Juvenile Courts." Illinois Courts. June 23, 2020. https://www.illinoiscourts.gov/News/388/Illinois-Supreme-Court-History-Juvenile-Courts/news-detail/
- Jane Addams Hull-House Association. "Jane Addams and Child Protection." n.d. Accessed December 3, 2025. https://janeaddamshullhouse.org/history/jane-addams-and-child-protection/
- Kanner, Leo. “The Psychopathological Problems of Childhood.” In Practical Clinical Psychiatry, 5th ed., edited by Edward A. Strecker, Franklin G. Ebaugh, and Leo Kanner. Philadelphia: The Blakiston Company, 1940. https://catalog.hathitrust.org/Record/002066736
- Rhoades, M. Carter. A Case Study of Delinquent Boys in the Juvenile Court of Chicago. Chicago: The University of Chicago Press, 1907. https://catalog.hathitrust.org/Record/001135857
Medical Treatments
- Abbott Laboratories. Abbott, Servant to Medicine. Chicago: Runkle-Thompson-Kovats, 1938. https://catalog.hathitrust.org/Record/001575765
- Ban, Thomas A. “Fifty years chlorpromazine: a historical perspective.” Neuropsychiatr Dis Treat 3, no. 4 (August 2007): 495-500. https://pmc.ncbi.nlm.nih.gov/articles/PMC2655089/
- Benzodiazepine Information Coalition. “A Brief History Of Benzodiazepines.” n.d. https://www.benzoinfo.com/a-brief-history-of-benzodiazepines/
- Freeman, Walter and James W. Watts. Prefrontal lobotomy in the treatment of mental disorders. Psychological Cinema Register, Pennsylvania State College, 1942. https://collections.nlm.nih.gov/catalog/nlm:nlmuid-8800490A-vid
- Freeman, Walter and James W. Watts. Psychosurgery: Intelligence, Emotion and Social Behavior following Prefrontal Lobotomy for Mental Disorders. Springfield, Ill.: Charles C. Thomas, 1942. https://catalog.hathitrust.org/Record/102194621
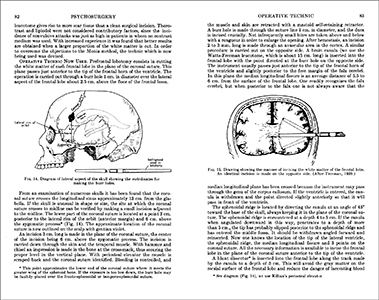
- Harlow, J.M. Recovery from the Passage of an Iron Bar through the Head. Boston: David Clapp & Son, 1869. https://collections.nlm.nih.gov/catalog/nlm:nlmuid-66210360R-bk
- Hillhouse, Todd M., and Joseph H. Porter. “A brief history of the development of antidepressant drugs: From monoamines to glutamate.” Exp Clin Psychopharmacol 23, no. 1 (February 2015): 1-21. https://pmc.ncbi.nlm.nih.gov/articles/PMC4428540/
- PharmaPhorum. “A history of the pharmaceutical industry.” September 1, 2020. https://pharmaphorum.com/r-d/a_history_of_the_pharmaceutical_industry
- Holland, Ryan, David Kopel, Peter W. Carmel, and Charles J. Prestigiacomo. “Topectomy versus leukotomy: J. Lawrence Pool’s contribution to psychosurgery.” Neurosurgical Focus 43, no. 3 (2017): E7 https://doi.org/10.3171/2017.6.FOCUS17259
- Ives, John. Electricity as a Medicine and Its Mode of Application. New York: Galvano-Faradic Mfg. Co., 1887. https://catalog.hathitrust.org/Record/100165997
- Journal of the American Pharmaceutical Association 1, no. 8 (1961): 491
- López-Muñoz, Francisco, Ronaldo Ucha-Udabe, and Cecilio Alamo. “The history of barbiturates a century after their clinical introduction.” Neuropsychiatr Dis Treat 1, no 4 (December 2005): 329-343. https://pmc.ncbi.nlm.nih.gov/articles/PMC2424120/
- Neurology 6, no. 11 (1956): 754.
- Orkaby, Asher and Sukumar P. Desai. “The Death of Sodium Pentothal: The Rise and Fall of an Anesthetic Turned Lethal.” J Hist Med Allied Sci 76, no. 3 (July 2021): 294-318. https://doi.org/10.1093/jhmas/jrab016
- Pow, Joni Lee, Alan A. Baumeister, Mike F. Hawkins, Alex S. Cohen, and James C. Garand. “Deinstitutionalization of American Public Hospitals for the Mentally Ill Before and After the Introduction of Antipsychotic Medications.” Harvard Review of Psychiatry 23, no. 3 (May/June 2015): 176-187. https://www.lsu.edu/hss/psychology/faculty/biological/SecondHarvardReviewPaper.pdf
- Rogers, Kara. "Insulin shock therapy". Encyclopedia Britannica. May 26, 2023. https://www.britannica.com/science/insulin-shock-therapy
- Wood Library Museum of Anesthesiology. “Magneto-Electric Machine.” Museum Collection, Alternative Medicine. https://www.woodlibrarymuseum.org/museum/magneto-electric-machine/
Chicago's Approach
- Adams, Dani. "Democratizing Mental Health." South Side Weekly (Chicago), February 4, 2020. https://southsideweekly.com/mental-health-advocates-put-public-services-back-on-table/
- Bradbury, J., M. Hutchinson, J. Hurley, and H. Stasa. "Lived Experience of Involuntary Transport under Mental Health Legislation." Int J Ment Health Nurs 26, no. 6 (Dec 2017): 580-92. https://doi.org/10.1111/inm.12284
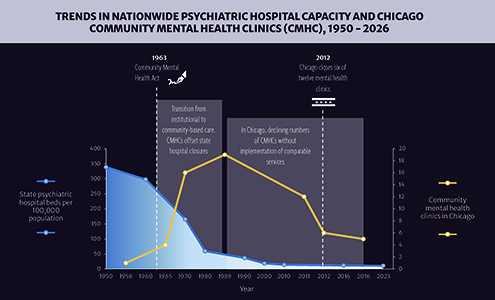
- Bradford, Shannon. "The History of Community Mental Health Care." The Chicago Policy Review (March 12, 2021). Accessed December 12, 2025. https://chicagopolicyreview.org/2021/03/12/community-mental-health-care-lessons-from-history/
- Brink, J., J. Livingston, S. Desmarais, C. Greaves, V. Maxwell, E. Michalak, R. Parent, S. Verdun-Jones, and C. Weaver. A Study of How People with Mental Illness Perceive and Interact with the Police. Mental Health Commission of Canada (Calgary, Alberta: 2011). https://mentalhealthcommission.ca/research/research/a-study-of-how-people-with-mental-illness-perceive-and-interact-with-the-police/
- Burke, Nancy, and Angela Sedeño. "The Kedzie Center: Community-Immersed Health from the Ground Up." Int J Appl Psychoanal Studies 20 (May 2023): 178-89. https://doi.org/10.1002/aps.1816
- City-State-Community Mental Health Task Force. City-State-Community Mental Health Task Force Report. [Chicago]: City-State-Community Mental Health Task Force, 1972.
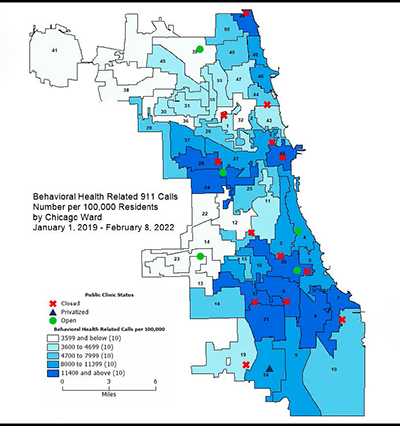
- Collaborative for Community Wellness. 911 Behavioral Health Call Rates Across Chicago’s Wards: Understanding Call Rates in the Context of Disinvestment in Public Mental Health Services. January 1, 2022. https://collaborativeforcommunitywellness.org/911-behavioral-health-call-rates-across-chicagos-wards-understanding-call-rates-in-the-context-of-disinvestment-in-public-mental-health-services/
- Erickson, Blake. "Deinstitutionalization through Optimism: The Community Mental Health Act of 1963." American Journal of Psychiatry Residents’ Journal 16, no. 4. (June 2021): 6-7. Accessed January 5, 2026. https://doi.org/10.1176/appi.ajp-rj.2021.160404
- Harcourt, Bernard E. "Reducing Mass Incarceration: Lessons from the Deinstitutionalization of Mental Hospitals in the 1960s." Ohio State Journal of Criminal Law 9, no. 1. (2011): 53-88. Accessed January 5, 2026. https://heinonline.org/HOL/P?h=hein.journals/osjcl9&i=55
- Lydersen, Kari. "‘Falling through the Cracks’." The Chicago Reporter, April 27, 2015. https://www.chicagoreporter.com/falling-through-the-cracks/
- McGhee, J., D. Brozost-Kelleher, I. Senechal, S. Stecklow, J. Mayzouni, A. Miglietta, and S. Ocneanu. "Shadow Arrests: Chicago Police Make Growing Use of Forced Psychiatric Hospitalization." South Side Weekly (Chicago), August 28, 2025. https://southsideweekly.com/shadow-arrests-chicago-police-make-growing-use-of-forced-psychiatric-hospitalization/
- Morrissey, Joseph P., and Howard H. Goldman. "Care and Treatment of the Mentally Ill in the United States: Historical Developments and Reforms." The Annals of the American Academy of Political and Social Science 484 (March 1986): 12-27. https://www.jstor.org/stable/1045181
- Musto, David F. "Whatever Happened to 'Community Mental Health?'" The Public Interest 39 (Spring 1975): 53-79. https://www.nationalaffairs.com/public_interest/detail/whatever-happened-to-community-mental-health
- Pilsen Little-Village Community Mental Health Center [flyer]. Tracy Baim Editorial Files, Windy City Box N (Alexander Street Press). LGBT Thought and Culture Database. Accessed 7 Jan. 2026.
- Sharfstein, Steven S. "Whatever Happened to Community Mental Health?" Psychiatric Services 51, no. 5. (May 2000): 616-20. Accessed January 6, 2026. https://doi.org/10.1176/appi.ps.51.5.616
- Smith, Michelle R. "50 Years Later, Kennedy’s Vision for Mental Health Not Realized." The Seattle Times, October 20, 2013. https://www.seattletimes.com/nation-world/50-years-later-kennedyrsquos-vision-for-mental-health-not-realized/
- Torrey, E. Fuller. Nowhere to Go: The Tragic Odyssey of the Homeless Mentally Ill. 2 ed. Springer Cham, 2025. https://doi.org/https://doi.org/10.1007/978-3-031-84685-4
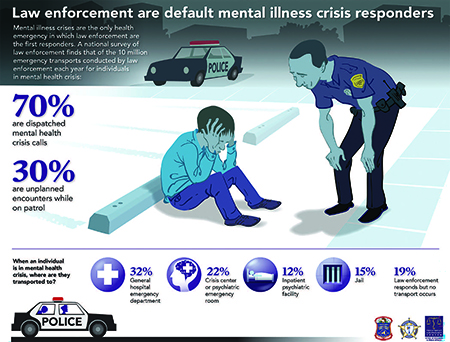
- Treatment Advocacy Center. Road Runners: The Role and Impact of Law Enforcement in Transporting Individuals with Severe Mental Illness, a National Survey. May 2019. https://www.tac.org/reports_publications/road-runners-the-role-and-impact-of-law-enforcement-in-transporting-individuals-with-severe-mental-illness/
- Watson, A. C., and J. D. Wood. "Everyday Police Work during Mental Health Encounters: A Study of Call Resolutions in Chicago and Their Implications for Diversion." Behav Sci Law 35, no. 5-6 (Sep 2017): 442-55. https://doi.org/10.1002/bsl.2324



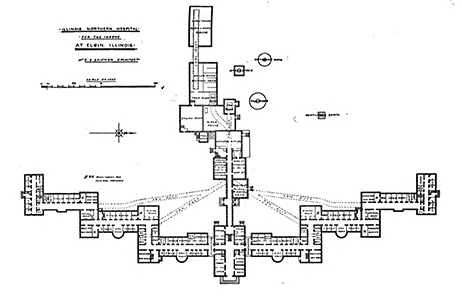
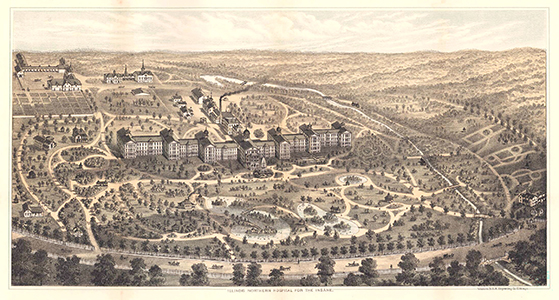







 Published in 1887,
Published in 1887,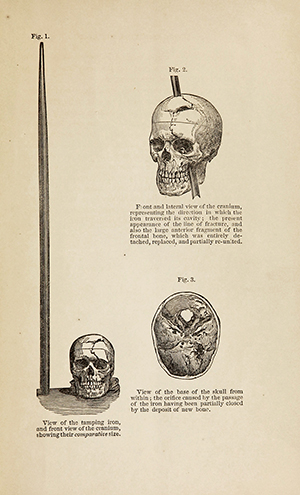 In 1848, Phineas Gage was working as a railroad construction foreman when an explosion drove a 3’ 7” long tamping iron through his face and head, destroying eyesight in his left eye, and much of his left frontal lobe. Though he survived, in subsequent years friends of Gage reported drastic changes in his personality, leaving him more volatile and sometimes violent. Dr. John M. Harlow detailed the injuries and behavioral changes in the above 1869 pamphlet. Incidences such as this clearly pointed toward the importance of the brain itself in controlling human behavior.
In 1848, Phineas Gage was working as a railroad construction foreman when an explosion drove a 3’ 7” long tamping iron through his face and head, destroying eyesight in his left eye, and much of his left frontal lobe. Though he survived, in subsequent years friends of Gage reported drastic changes in his personality, leaving him more volatile and sometimes violent. Dr. John M. Harlow detailed the injuries and behavioral changes in the above 1869 pamphlet. Incidences such as this clearly pointed toward the importance of the brain itself in controlling human behavior.